Are you interested in learning more about the COVID-19 vaccine? Please see the Vaccine Information page.
While vaccines reduce the spread of COVID-19, continuing to use contact tracing can reduce the spread also. By using multiple tools to reduce spread, we can have a bigger effect on limiting the virus. Our goal is to keep the virus from spreading by limiting the number of people it can infect.
The Oregon Health Authority has provided a guide explaining COVID-19 test results, which can be obtained here.
Novel coronavirus, or COVID-19, is a new coronavirus that is different than the other coronaviruses that have been previously identified; therefore, information and recommendations may change as new data becomes available. Please check back for updated information.
COVID-19 symptoms include cough and shortness of breath or at least 2 of the following symptoms: fever or chills, cough, shortness of breath or difficulty breathing, fatigue, muscle or body aches, headache, new loss of taste or smell, sore throat, congestion or runny nose, and diarrhea. It may take up to 2 or as long as 14 days after exposure to the virus for symptoms to appear. Most people will have mild symptoms but some will experience more severe symptoms.
COVID-19 is spread from person-to-person. Risk increases between people who are in close contact with each other (within 6 feet). When an infected person talks, sneezes or coughs, respiratory droplets are released into the air and these droplets can land in the mouth, nose, or eyes of people who are nearby or be inhaled into the lungs. COVID-19 may be spread by people who are not showing symptoms.
COVID-19 is thought to be more contagious than the flu, but less contagious than measles, which is highly contagious. The more closely a person interacts with others and the longer that interaction, the higher the risk of passing on the infection.
While not the main source of infection, it may be possible that COVID-19 transmits by touching a surface or object that has the virus on it and then touching the mouth, nose or eyes.
Risk increases steadily with age. People of any age with the following conditions are at increased risk for severe illness from COVID-19:
- Chronic kidney disease
- COPD (chronic obstructive pulmonary disease)
- Immunocompromised state (weakened immune system) from solid organ transplant
- Obesity (body mass index [BMI] of 30 or higher)
- Serious heart conditions, such as heart failure, coronary artery disease, or cardiomyopathies
- Sickle cell disease
- Type 2 diabetes mellitus
Children who are medically complex, who have neurologic, genetic, metabolic conditions, or who have congenital heart disease are at higher risk for severe illness from COVID-19 than other children.
Based on what we know at this time, people with the following conditions might be at an increased risk for severe illness from COVID-19:
- Asthma (moderate-to-severe)
- Cerebrovascular disease (affects blood vessels and blood supply to the brain)
- Cystic fibrosis
- Hypertension or high blood pressure
- Immunocompromised state (weakened immune system) from blood or bone marrow transplant, immune deficiencies, HIV, use of corticosteroids, or use of other immune weakening medicines
- Neurologic conditions, such as dementia
- Liver disease
- Pregnancy
- Pulmonary fibrosis (having damaged or scarred lung tissues)
- Smoking
- Thalassemia (a type of blood disorder)
- Type 1 diabetes mellitus
The best way to protect yourself and others is to avoid exposure to the virus.
- Limit contact and stay 6 feet away from people you do not live with.
- Wash hands often with soap and water for 20 seconds. If that is not available, use hand sanitizer that contains at least 60% alcohol.
- Avoid touching your eyes, nose and mouth with unwashed hands.
- Avoid contact with people who are sick.
- Stay home while you are sick, except to seek medical care, and avoid close contact with others.
- Wear a cloth face covering to cover mouth and nose when going into a public setting (i.e. grocery store).
- Cover your mouth and nose with a tissue or sleeve when you cough or sneeze.
- Clean and disinfect frequently touched surfaces daily. This includes door handles, countertops, light switches, phones, toilets, keyboards and remote controls.
- If you are at risk for severe complications (older than age 65 or have medical conditions) you should stay home, even if you feel well.
Call Before You Go
Most people can recover at home without the need for medical services. If you think that you need medical assistance call the clinic or Emergency Department BEFORE you go in and tell them your symptoms. This will allow staff to evaluate your condition and instruct you on how to enter the building. If you notice any of the following symptoms, seek medical attention immediately:
- Difficulty breathing or shortness of breath
- Persistent pain or pressure in the chest
- New confusion or inability to rouse
- Bluish lips or face
The Baker County Health Department is asking people with symptoms to stay home if they are not ill enough to seek medical attention. If you need medical attention, please contact your medical provider or the Emergency Department BEFORE you go in and tell them your symptoms to be assessed and get instructions of how to enter the facility. A medical provider will decide if you need tested for COVID-19.
St. Alphonsus Information:
With the increase in COVID-19 cases, Saint Alphonsus Medical Center would like to remind people with mild symptoms to stay home if they would not normally seek medical attention. If you are experiencing mild to moderate symptoms consistent with COVID-19, please call the clinic at 541-524-8000 and schedule an appointment to be seen. The clinic will take appointments 7am-noon and 1-4pm Monday through Friday. If you are experiencing any of the following symptoms, seek medical attention at the Emergency Department or call 911 immediately:
- Difficulty breathing or shortness of breath
- Persistent pain or pressure in the chest
- New confusion or inability to rouse
- Bluish lips or face
St. Luke’s EOMA Information:
St. Luke’s EOMA is open Monday through Friday from 7-5 for scheduled appointments either through telemedicine or face-to-face encounters. We are open Monday through Friday 8-4 and Saturday 8-12 for walk-in clinic. For patients with symptoms of fever, cough, shortness of breath, and/or GI issues, we will send an MA/Provider out to your car. If a patient would like to schedule an appointment for pre-travel or asymptomatic COVID testing, they will need to do so through MyChart. For all other COVID testing, call our main number listed below to get scheduled. For other acute issues we are putting those on open schedules when available, if no appointments are open at that time we can see those patients in the building at our walk-in clinic. Moderna or Johnson & Johnson COVID vaccines are available during open hours, please call to schedule. We have a strict masking protocol that asks each patient to wear a procedure mask while inside the building. Our visitor policy is currently allowing 2 adults for a child’s appointment, 1 visitor for obstetric appointments, or 1 visitor for adult appointments (this includes a care giver). Please call our main number at 541-523-1001 and we will help you get the appropriate appointment set up. We provide individuals with medically qualified Interpreters. Cultural and Language Services offers Video, Phone and In-Person Interpretation resources to ensure 24/7/365 support. We provide Interpretation and Translation services to individuals at no cost.
Follow these links for more information:
Centers for Disease Control and Prevention
https://www.cdc.gov/coronavirus/2019-ncov/index.html
Oregon Health Authority
https://govstatus.egov.com/OR-OHA-COVID-19
Johns Hopkins University & Medicine Interactive Map
https://coronavirus.jhu.edu/map.html
July 2021 Archives:
With the increase in COVID-19 cases, and the unfortunate report of the first COVID-19 related death in Baker County, Saint Alphonsus Medical Center would like to remind people with mild symptoms to stay home if they would not normally seek medical attention. If you are experiencing mild to moderate symptoms consistent with COVID-19, curbside assessment is available on the backside of the physician’s clinic, off of Midway Drive, from 8:00 am to noon and from 1:00 pm to 4:00 pm Monday through Friday. If you are experiencing any of the following symptoms, seek medical attention at the Emergency Department or call 911 immediately:
April 2021 Archives:
The Oregon Health Authority has developed a website specifically related to this vaccine, along with a handout answering frequently asked questions.
The Baker County Health Department is scheduling COVID-19 vaccines for those aged 12 and older. The Moderna and Johnson & Johnson vaccines are available for those aged 18 and older, while Pfizer is available for those 12-17 years old. The best way to get scheduled for a vaccine is by signing up online (COVID-19 vaccine sign up form) and our staff will call to schedule your appointment or you can call 541-523-8211.
Vaccines are also available through our community partners at Rite Aid, Bi-Mart, Safeway, Albertsons, St. Alphonsus and St. Luke’s EOMA.
Those who have received their vaccines in other states are encouraged to bring their vaccine records to the Health Department so we can put them in ALERT, our state’s immunization system. You can bring all immunization records (childhood and/or COVID-19). This benefits families by having all of their vaccines in one system so they can easily get copies of their records when needed. Regarding COVID-19 vaccines, it also helps our county reach our goal of 65% of those 16 years and older being immunized.
If you have questions regarding the COVID-19 vaccine or COVID-19 in general, please contact the Baker County Health Department at 541-523-8211. We are happy to answer any questions you may have.
- Fact Sheet for Moderna Vaccine EUA
- Fact Sheet for Pfizer Vaccine EUA
- Fact Sheet for Johnson & Johnson Vaccine EUA
The Baker County Health Department is administering COVID-19 vaccines in accordance with OHA’s Vaccine Sequencing Plan, included below. The best way to get scheduled for a vaccine is by signing up online using this link: COVID-19 vaccine sign up form or by calling 541-523-0015. If no one answers, please leave a message and someone will call you back. Once on the list, you may be contacted by one of our community partners as vaccine is available, including a pharmacy or the hospital. If you are already on the list at the Health Department and have received your vaccine from another location, please call and let us know so we can schedule others who still need the vaccine.

February 2021 Archives:
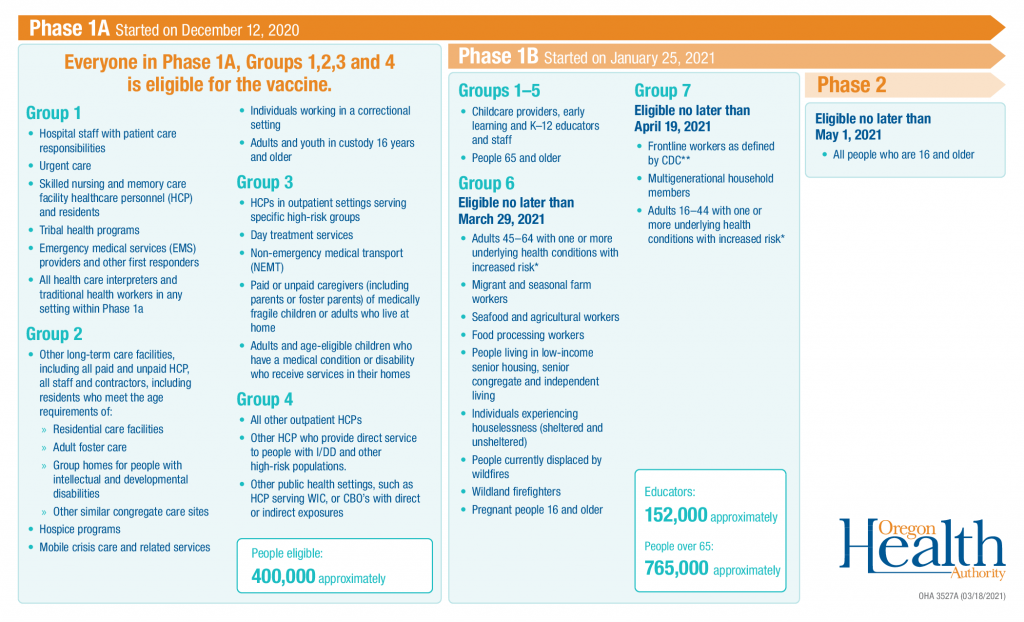
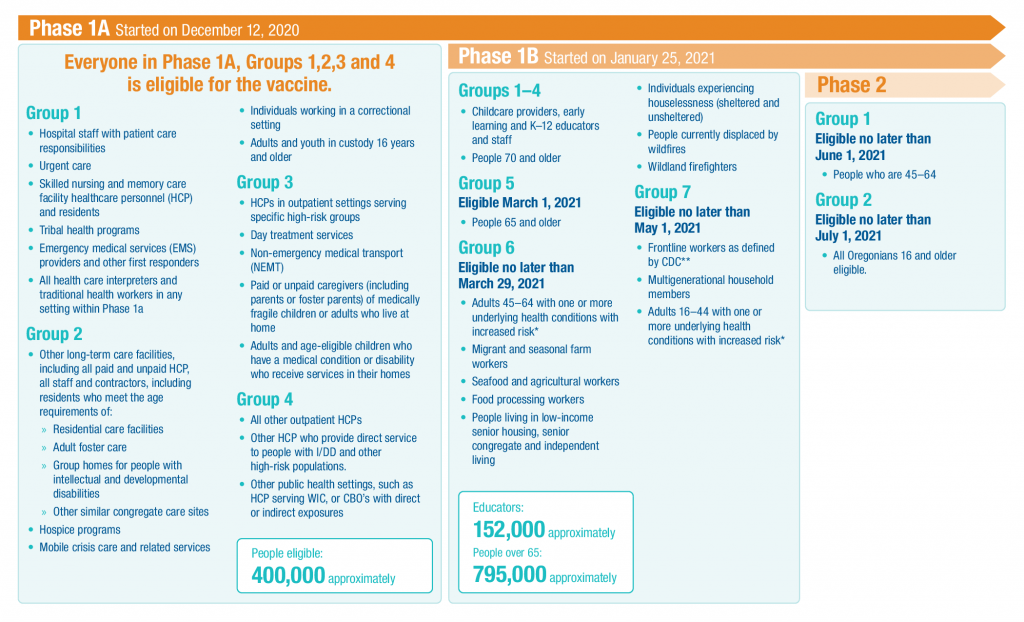

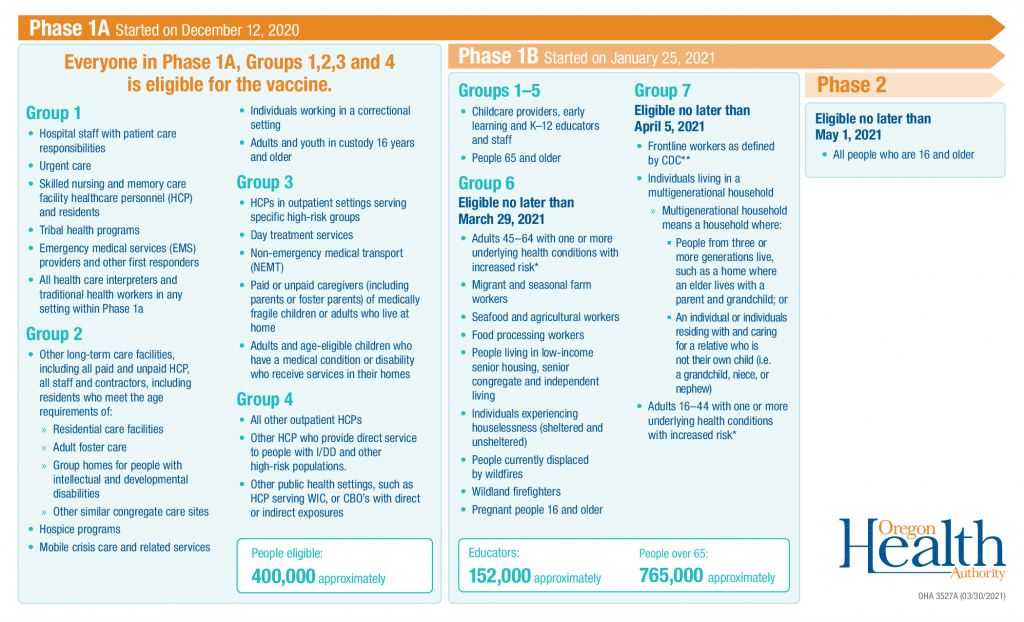
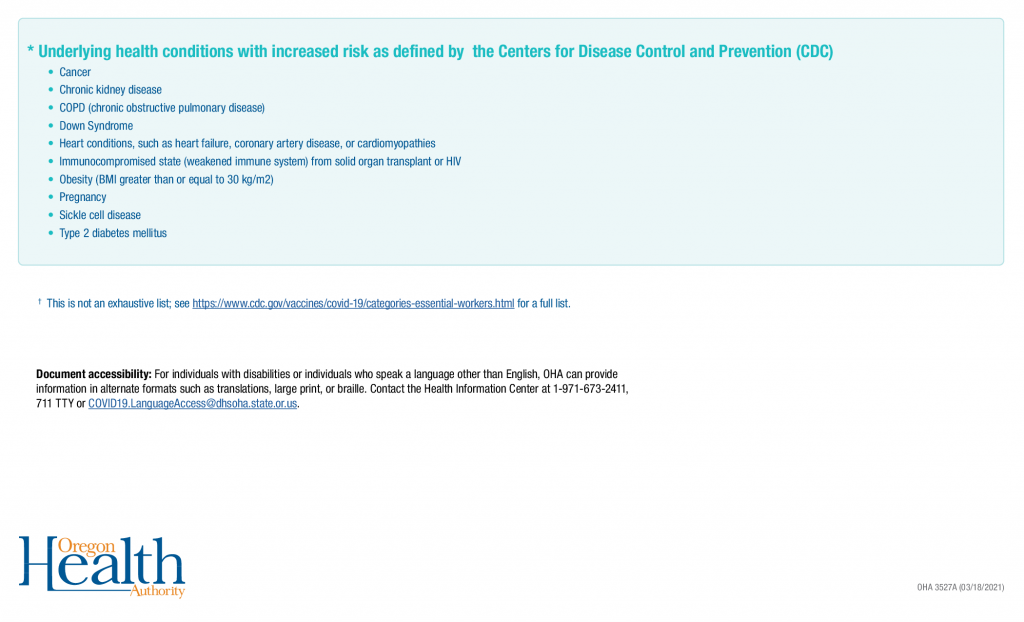
As vaccines are being distributed throughout the state, the Baker County Health Department will be administering vaccines in accordance with OHA’s Vaccine Sequencing Plan, which prioritizes high risk groups. As vaccines become available to these groups, information will be updated here. Other information can also be found on the Baker County Oregon Health Department Facebook page or be included in press releases for local publications. The Baker County Health Department welcomes questions by phone at 541-523-8211 and appreciates your patience as we adapt to rapidly changing information and vaccine availability.
Thank you for all of the great questions about getting vaccinated. We are working to keep everyone informed as we learn more about availability, and appreciate your patience as we work towards vaccinating all of our community members that want to get the vaccine. Please continue to check our website as we will be continuing to add COVID-19 Vaccine distribution events and populations served. Currently, our vaccine distribution events are by appointment only. You will receive a call to schedule an appointment when we reach your turn on our waiting list. We encourage you to answer your phone and check messages so that you do not miss our call.
We are currently working on all groups in Phase 1A (described below in the blue highlighted area) and 1B Groups 1, 2 and 3 (described below in the yellow highlighted area). Those aged 18 or older are encouraged to sign up using our call center, which will be open Monday through Friday from 8am-12pm and 1:30pm-5pm, by calling 541-523-0015. If no one answers, please leave a message and we will call you back. You can also sign up by using this online link: COVID-19 vaccine sign up form.
The Baker County Health Department will call to schedule your appointment when vaccine becomes available for your age group. Our vaccine supply may not keep up as additional groups open. If you are on our wait list, we will call you to schedule an appointment as soon as vaccine is available.
Phase 1A Group Descriptions are as follows:
Group 1: Hospitals; urgent care; skilled nursing and memory care facility HCP and residents; tribal health programs; EMS providers and other first responders
Group 2: Other LTCFs and congregate care sites including HCP and residents; hospice programs; mobile crisis care and related services; secure transport; individuals working in a correctional setting
Group 3: Outpatient settings serving specific high-risk groups; in home care; day treatment services; non-emergency medical transport (NEMT)
Group 4: HCP in other outpatient, public health and early learning settings; death care workers
Phase 1B Group Descriptions are as follows:
Group 1: Childcare providers, early learning and K-12 educators and staff are eligible the week of January 25, 2021
Group 2: People 80 and older are eligible the week of February 7, 2021
Group 3: People 75 and older are eligible the week of February 14, 2021
Group 4: People 70 and older are eligible the week of February 21, 2021
Group 5: People 65 and older are eligible the week of February 28, 2021
Vaccines are not available for anyone under the age of 18. Please continue to check back for more information. We will continue to update this information as it becomes available.
We appreciate your patience as our phones are ringing off the hook (we share your excitement)! If you call the Health Department and reach our voicemail, please leave a message. We are checking voicemail regularly and will call you back. Continue to watch our Facebook page (Baker County Oregon Health Department) and this website for updates. More information can also be found at https://covidvaccine.oregon.gov/.
January 2021 Archives:
Vaccination of Oregon seniors, educators to begin January 23, pending increased vaccine deliveries from the federal government. We will continue to update on availability as we learn more.
December 2020 Archives:
We are currently vaccinating eligible individuals under Phase 1A, Groups 1-4. Please contact the Baker County Health Department if you are interested in getting scheduled for your COVID-19 Vaccine.
August 2020 Archives:
In Oregon, testing supplies are limited at this time. Testing is being conducted locally by medical providers for those that meet testing criteria.
Oregon Health Authority recommends that any person with symptoms consistent with COVID-19 be tested for COVID-19.
If resources are limited, people with symptoms in the groups listed below should be prioritized. Severity of symptoms and available testing and health care system capacity should be factored into the decision, including staff, PPE, testing supplies, specimen collection supplies and current testing turnaround time.
- Healthcare workers and first responders (EMS, public safety workers)
- Residents, staff, children, or other people in a care facility or group living setting (e.g., healthcare facility, residential care facility, school, agricultural workers, food-packing plants, child care, corrections, shelters, etc.).
- Workers who provide direct care of service in multiple group facilities or who provide in-home services (e.g., hospice care workers, physical or occupational therapists, in-home personal care workers, etc.)
- Essential front-line service workers who have regular contact with large numbers of people (e.g., those working in grocery stores, pharmacies, food service, transportation, delivery, and other critical infrastructure services)
- Patients 60 years of age or older
- Patients with underlying medical conditions, including, but not limited to hypertension, diabetes, cardiovascular disease, lung disease, and immunocompromising conditions
- People who identify as Black, African-American, Latino, Latina, Latinx, American Indian/Alaska Native, Asian, Asian-American or Pacific Islander
- People who identify as having a disability
- People whose first language is not English
- Pregnant women
- Patients whose condition requires hospitalization
- Patients who within 14 days of their symptom onset had close contact with a person with laboratory-confirmed COVID-19 or a person determined by a publish health authority to be a presumptive case
OHA recommends that testing of people without symptoms consistent with COVID-19 be limited to the following groups: a. Close contacts of a person with laboratory-confirmed COVID-19 or of a person determined by a public health authority to be a presumptive case, b. People exposed to COVID-19 in a congregate setting, c. Migrant/seasonal agricultural workers upon arrival in Oregon, d. People who identify as Black, African-American, Latino, Latina, Latinx, American Indian/Alaska Native, Asian, Asian-American or Pacific Islander, e. People who identify as having a disability, and f. People whose first language is not English.
July 2020 Archives:
Saint Alphonsus has provided an updated schedule regarding their curbside clinic. As of April 29, 2020, the curbside assessment was moved to the parking lot behind the physician’s clinic to the right of the Emergency Department parking lot. It will be operational from 8:00 am to noon and 1:00 pm to 4:00 pm Monday-Friday.
March 2020 Archives:
Saint Alphonsus has provided an updated schedule regarding their curbside clinic, which can be obtained here. As of April 10, 2020, the curbside assessment was moved to the parking lot behind the physician’s clinic to the right of the Emergency Department parking lot. It will be operational from noon to 4:00 pm Monday-Friday.